
Joanne appears on the “What next?” podcast with Kirsty Robbie
20 Dec 2022
Treating People Not Symptoms – From Pharmacist to Naturopath
13 Nov 2023
What is AMH?
Anti-Mullerian hormone (AMH) is a hormone that is produced predominantly by the actively growing follicles within the granulosa cells of the ovary. These follicles are the smallest, earliest stages of growth and development of the follicle or egg.
Your AMH Level is a reflection of your growing follicles.
Your AMH level is a reflection of your growing or actively maturing follicles.
In other words, your AMH level reflects the pool of growing follicles that can potentially ovulate at a given time during your menstrual cycle.
It is NOT a measure of the number of eggs you have left, nor the quality of your eggs, but rather a way of assessing your ‘functional ovarian reserve’ i.e. the potential number of follicles available to be recruited.
This functional ovarian reserve constitutes the pool of follicles 2-5mm in diameter from which 1 follicle is destined to be selected and to ovulate. This pool of growing follicles is known as the AMH-producing follicles.
Your AMH level increases until early adulthood, peaks at about 25 years of age, and then slowly declines until after menopause (at which time there are no more actively growing follicles).
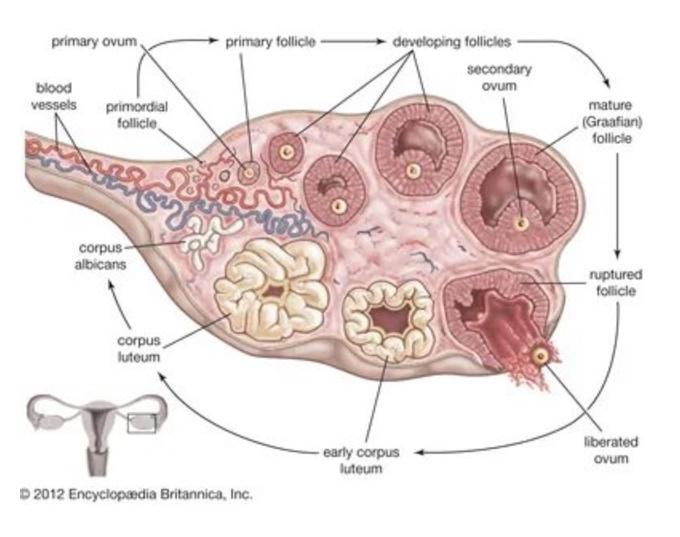
Cycle of maturing egg within the ovary – from recruited follicles to ovulation
What is your AMH Level?
If you have a Low AMH level, it means that you have fewer growing follicles and at that moment in time, your functional ovarian reserve is low…..it does NOT mean you are ‘running out of eggs’!
Women who genetically have low AMH levels will still be able to produce a dominant follicle that will mature and ovulate – thus they will be able to conceive – even though they had fewer growing follicles than women of similar age with normal AMH levels.
Your AMH level naturally starts to decrease with age, but you should still be able to conceive. The issue is that there are even fewer follicles to recruit, so it might become more difficult the older you get.
If you have a High AMH level, you more than likely have PCOS (Polycystic Ovarian Syndrome).
Your ovaries are densely packed with follicles. You have a large number of follicles that are available to be recruited. But because the ovaries are so chock-full, there’s not enough space for any of them to grow and form at least one mature, dominant follicle. Therefore ovulation doesn’t occur.
Your AMH level shows ovarian density. So the higher your AMH above the normal for your age, the lower your chances of ovulating.
How do AMH levels relate to your Fertility?
According to research, AMH levels are ‘not a good predictor of female fertility’!
‘AMH measurement is only useful as an indirect marker of the remaining female fertile years in those women who have premature ovarian failure.‘
The American Journal of Reproductive Medicine Fertility and Sterility Journal Review discusses a very recent paper on the clinical use and misuse of AMH in current reproductive medicine practice – quote:
“… using AMH to forecast fertility potential can be fraught with error and can drive unwarranted medical treatment. Certain conditions and medications can also result in falsely low AMH determinations, which can again lead to inappropriate treatment recommendations. The knowledge of the proven usefulness of AMH and its limitations is therefore critical for optimal clinical practice.”
Among women aged 30-44, without a history of infertility who had been trying to conceive for 3 months or less… ‘findings do not support the use of AMH levels to assess natural fertility with these characteristics’.
AMH is NOT a fertility check
[Listen – 6 mins]
Markers of ovarian reserve as predictors of future fertility
Excerpt from “Fertility and Sterility On Air – TOC: January 2023”
Is AMH important for IVF treatment?
Fertility specialists are interested in measuring AMH levels as it helps them decide which assisted reproductive technique, ovarian stimulation protocol, and medication dosage they will use for the IVF cycle.
It has nothing whatsoever to do with predicting the quality of your eggs during egg retrieval.
In other words, if you are undergoing IVF, your specialist would need to work out if you have enough actively growing follicles for a successful outcome during that cycle, and also how well your ovaries will respond to being stimulated with medication.
In these cases, women with low AMH levels might need their stimulation medication adjusted accordingly. And women with high AMH levels, as in PCOS, would need to be carefully monitored.
What factors other than age could cause low AMH levels?
- Smoking – affects ovarian function as well as the quality of the eggs.
- Endocrine Disruptors – Environmental toxins affect ovarian function and quality of the eggs in a similar way to smoking.
- BMI – Being Over or underweight are both problematic for ovarian function and therefore AMH.
- Contraceptive use – this will decrease AMH levels by 30-40%. So it’s pointless testing for AMH during contraceptive use. Best to wait at least until at least 3 months of coming off contraception before you do the AMH test.
- Low Vitamin D levels – chronically low level of vitamin D has been known to compromise AMH. Higher AMH levels have been reported during Summer than Winter.
- Premature Ovarian Insufficiency – This occurs when the ovaries aren’t functioning well. They don’t produce enough oestrogen to be able to ovulate regularly.
- Ovarian surgery
- Genetic factors
Are AMH levels changeable in some women?
Yes!
Your AMH levels can change during various times of your cycle and under certain conditions.
As you’ve seen in the above examples, hormonal, seasonal, genetic and epigenetic (lifestyle) factors can all influence your AMH levels.
There are many avenues I use in my practice to help women improve their health status and hence their AMH levels.
Is there anything that can help improve AMH levels?
Even though there are no medical options available for improving AMH status, naturopathically there are many.
As a Naturopathic Fertility Practitioner, I consider AMH levels as just one part of a much bigger picture when making my overall assessment of each patient. I consider many factors when giving advice and making my treatment decisions.
Some examples of my natural approach to improving your AMH levels:
- During the consultation I would explain my ‘4 Steps to Fertility’ protocol. This includes advice on a good ‘fertility improvement’ diet as well as lifestyle factors such as exercise, relaxation and avoidance of endocrine disrupting chemicals. The advice I give is fully backed by research and studies that are known to improve fertility as well as AMH levels.
- I might also suggest certain supplements such as Vitamin D, Iron, Zinc etc. (if your levels don’t fall into my optimal fertility values range).
- I often prescribe antioxidants and fish oil as these are known to be beneficial too.
- Appropriate herbal medicines are extremely important for addressing hormonal imbalance which usually influence your overall fertility as well as your AMH levels.
I hope I have given you a better understanding of AMH and how I approach it from a naturopathic perspective.
I also hope I’ve given you more confidence in your fertility prospects regardless of what your levels are.
Joanne Lipinski – Fertility Naturopath Melbourne
Related Link
Markers of ovarian reserve as predictors of future fertility
“Benjamin S. Harris M.D., M.P.H. , Anne Marie Jukic Ph.D. , Tracy Truong M.S. , Caroline T. Nagle M.P.H. ,
Alaattin Erkanli Ph.D. , Anne Z. Steiner M.D., M.P.H.”
